Umbilical cord infection in newborn baby…
March 2023
In the previous journey, I gave you information about how the umbilical cord is formed, how to care for the newborn umbilical cord, and the treatment of umbilical granuloma. In this course, I will tell you about the umbilical infection that can be seen in newborn babies.
Immediately after birth, the navel begins to be invaded by thousands of microorganisms. And as a matter of fact, the umbilical cord residue, which has begun to lose its vitality, creates a super suitable environment for bacteria to reproduce. Through the vessels in the cord, these bacteria have the potential to mix with the newborn baby’s blood and cause sepsis.
Infection of the umbilical cord and surrounding tissues is called “omphalitis”. It can show itself with discharge from the umbilical cord, swelling, tenderness and redness in the surrounding tissue. Fortunately, in developed countries, I think we can still put our country in this category, the incidence of omphalitis is about seven per thousand. But unfortunately, in some places, this rate can go up to 8 percent for those born in hospitals and 22 percent for those born at home. The use of antiseptics in such areas reduces the possibility of omphalitis and death due to omphalitis. I gave information about umbilical cord care in the previous cruise.
Which babies are at risk of getting a navel infection?
Low birth weight, prolonged delivery, early rupture of the membranes of the mother, if mother has infection, delivery in non-sterile environments, having to insert a catheter through the umbilical cord, and home birth increases the risk of omphalitis. Not caring for the umbilical cord properly, still applying traditional ash and manure applications, needless to say, invites infection anyway. No matter what we do, the baby may have a predisposition too. For example, in some cases of immune system failure, the risk of umbilical infection increases.
What happens when you have a navel infection?
A slight discharge, even a slight odor, is normal if the inflammatory signs I mentioned above are not accompanied by redness, swelling, tenderness, and fever. For example, a lot of umbilicus like you can see in the photo, are being consulted. After the cord falls off, the yellowish layer there and the slight yellowish discharge caused by that layer are completely normal. But if there is redness around the umbilical cord, infection may be starting. A slight bleeding is also normal with the delay of coagulation of the vessels in the navel. But I repeat, malaise, restlessness, fever, malnutrition are bad signs.
What can an umbilical cord infection cause?
The most important is the mixing of bacteria into the blood, namely sepsis, then inflammation and obstruction of the veins and the portal vein leading to the liver, liver abscesses, infection of the peritoneum, intestinal problems, infection of the abdominal wall, necrotizing fasciitis and death. The death rate is quite high at 7-15%. The outcome is worse for baby boys, home births, premature births, and babies with high fever.
How do we treat?
First, we definitely take a culture from the discharge. If there are systemic findings, sampling from blood and cerebrospinal fluid may be required. Of course we start antibiotics. It usually takes about 10 days of treatment. Local antiseptic and antibiotic creams can also be given, but their effectiveness is not as strong as intravenous antibiotics. We even recommend intravenous antibiotics, instead of oral route.
If the serious infection of the abdominal wall, which we call necrotizing fasciitis, gets involved, there is a significantly high mortality rate. In this case, the skin, subcutaneous, fat, and fascia layers become infected.
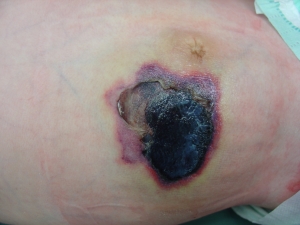
As you can see in the photo, the redness begins to turn black as the tissues begin to die. Infection and inflammation progress very rapidly, high fever occurs, bacteria mix with the blood and spread to the whole body, shock and then the loss of the baby occurs. We try to intervene very quickly. We clean the infected tissues in surgery and give a wide range of effective antibiotics and supportive treatment. Still, the infant mortality rate in necrotizing fasciitis cases reaches up to 60-85%.
It is best that we ensure that babies are delivered in clean environments, in hospitals, by health professionals who have received the necessary training, and instead of the traditional methods we heard from our elders, let’s do navel care as described by our doctors.
Everything for babies.
Prof. Dr. Egemen Eroğlu
March 2023


